Cycle Syncing vs Birth Control
What the Science Actually Says (and What It Doesn't)
I started this deep dive expecting to emerge with a plan: how to align my workouts, meals, and moods to my menstrual cycle–how to “get in tune” with my hormones and live more naturally. After all, that’s the sell on cycle syncing: that natural = right.
Right?
Well, maybe.
But first, what exactly is cycle syncing? Where did it come from? How does one cycle sync? Does it actually work?
And once you start asking those questions, others may follow: How does it compare to hormonal birth control? Is one healthier or safer than the other? And what does science–not influencers–actually say?
I’m not here to sell or bash either wellness trends or birth control. I’m here to understand how much of this is science and how much is wishful thinking because, like most of us, I just want to make informed choices about my body.
What in the Heck is Cycle Syncing?
Cycle syncing is a lifestyle approach (for those of us with a uterus) that involves aligning your daily habits (exercise, nutrition, work, and rest/recovery) with the four phases of your menstrual cycle.
The idea is that since hormone levels (mainly estrogen, progesterone, and testosterone) fluctuate throughout the month, your mood, metabolism, and focus also naturally shift.
The goal of cycle syncing is to work with, rather than against, those hormonal rhythms. For example, doing high-intensity workouts when estrogen and energy are high, and focusing on recovery when progesterone rises.
Where did it come from?
The scientific/biological basis (that hormones affect mood, metabolism, and energy) is well-established in endocrinology and reproductive physiology. 1
The term “cycle syncing” was coined by Alisa Vitti, a functional nutritionist and author of WomanCode and In the FLO. Her Cycle Syncing Method pairs diet, exercise, and productivity strategies with each hormonal phase. Since then, the idea has exploded across social media and wellness platforms, though its scientific foundation remains debated.
How does one cycle sync?
Let’s start with a quick breakdown of an average menstrual cycle.
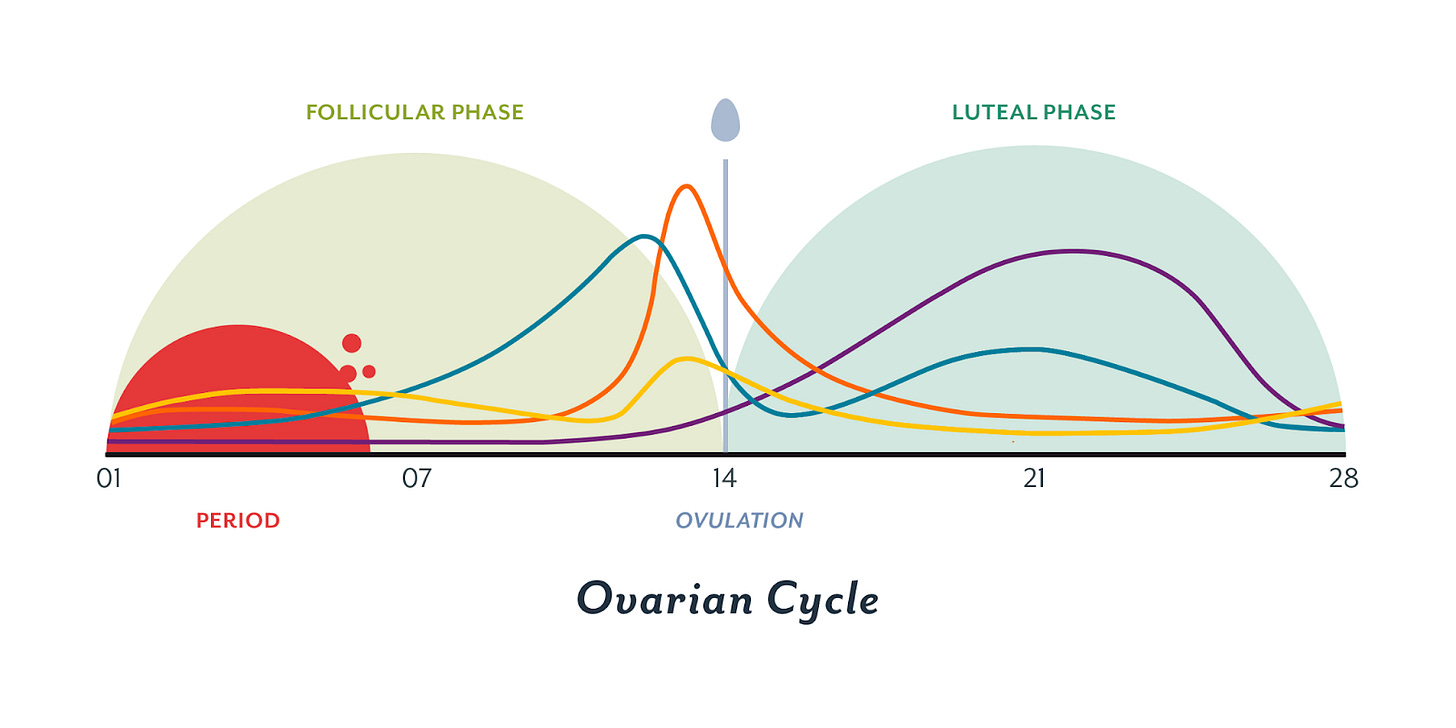
There are four phases in a cycle: luteal, follicular, menstrual, and ovulation. During each phase, hormonal levels increase and drop accordingly, which could have an impact on how you feel (pain tolerance, energy levels, and mood). Below is a cute little diagram I found2 that outlines how hormones are fluctuating throughout an average 28-day cycle.
And a key: Estrogen is teal, Progesterone is purple, LH is orange, FSH is yellow
There can be a lot of nuance to each phase and it is by no means super simple, but I am going to do my best to keep this easy breezy.
At a very simple level, you have two main phases, Follicular and Luteal. The Menstrual Phase marks the start of the Follicular phase which continues until ovulation. At which point the Luteal phase begins. This is nicely pictured above. A lot of sources will break the cycle into four phases. Because each phase is likely going to feel fairly unique, I will explain the cycle in four phases as well. Additionally, I have seen each phase related to a different season, so I will explain that.
Menstruation (Days 1-5/7)
Season: Winter
Overview: Uterine lining sheds, resulting in bleeding as hormone levels (estrogen and progesterone) are at their lowest
Activities: think restoration–yoga, walking, light cardio, light strength training
Food: raspberry leaf tea, warm stews and broths (mineral rich), seafood and pasture raised meats (want stuff high in omega 3s and vitamin B12)
Follicular Phase (Days 6/8)
Season: Spring
Overview: The pituitary gland releases FSH, stimulating follicles in the ovaries to mature and increasing estrogen to rebuild the uterine lining
Activities: cardio, HIIT towards the end of the phase, boxing, running, swimming
Food: colorful vegetables (stir frys and salads); prioritize fiber, fermented foods, and foods high in zinc
Ovulation (Day 14)
Season: Summer
Overview: A surge in LH triggers the release of an egg from the ovary, marking the most fertile period
Activities: even higher intensity than follicular, HIIT and cardio
Food: high quality nutrition like raw and crunchy veggies full of fiber, teas (dandelion root, turmeric, or milk thistle to flush estrogen) (ginger, peppermint, or fennel for bloating and cramping)
Luteal Phase (Days 15-28)
Season: Autumn
Overview: The corpus luteum produces progesterone to prepare the uterus for possible implantation; if pregnancy doesn’t occur, hormone levels drop and menstruation begins again
Activities: strength train with intention on form as you’re more likely to get hurt during this phase3 and low intensity cardio like pilates, barre, and yoga
Food: focus on blood sugar stability–foods high in fiber, vitamin B, magnesium, calcium; warm complex carbs; healthy fats (walnuts, avocados)
If you’re looking for even more information, the Balanced Beyars sisters are a great resource. They explain that when starting out, tracking your cycle using an app like MYFLO can be very helpful in addition to checking Basal Body Temp and Cervical Mucus.
It is also worth noting that it can take up to three months to feel the effects of cycle syncing.4
At this point, it all sounds pretty convincing, right? The biology checks out, the phases seem logical, and plenty of people have written detailed guides on how to sync your life to your cycle. But then I had to stop and ask: okay, this feels legit, but is it actually proven? How much of this is science-backed and how much is just smart-sounding theory? What does the research actually say?
Does cycle syncing work?
The hormonal basis of cycle syncing is legitimate; our estrogen, progesterone, and testosterone levels fluctuate in predictable ways, influencing mood, metabolism, and energy. But the evidence for specific lifestyle outcomes (improved productivity, fat loss or muscle gain, or athletic performance) remains limited.
Research in endocrinology supports that hormone fluctuations across the menstrual cycle influence measurable physiological and psychological factors like:
Basal body temperature and metabolism
Insulin sensitivity and energy use
Neurotransmitters (e.g. serotonin, dopamine) affecting mood and focus
Exercise performance and recovery patterns
But, whether we should adjust our workouts, diets, or productivity based on these changes remains fuzzy. Rigorous studies validating “cycle syncing” as a comprehensive system–as often presented by influencers or wellness apps–are scarce. Most experts agree that Cycle Syncing is best viewed as a framework for body awareness, not a scientifically standardized protocol.
Cycle Phase and Performance
Across studies, scientists have looked for consistent differences in strength, endurance, or recovery between menstrual cycle phases–and the results are lacking.
McNulty et al., 2020 (Sports Medicine, meta-analysis): Reviewed 78 studies and concluded that while small performance fluctuations exist across the cycle, large individual differences limit generalizations.5
Colenso-Semple et al., 2023 (Frontiers in Sports and Active Living): Current evidence shows no meaningful effect of menstrual-cycle phase on strength or training adaptations.6
Elliott-Sale et al., 2021 (Sports Medicine): Highlighted why so many studies are under-powered or poorly controlled–making bold “phase-based” training advice scientifically shaky.7
Harvard Apple Women’s Health Study update, 2025: Using app-based data from thousands of women, researchers found enormous interest in cycle syncing but insufficient evidence to prescribe training by phase. Individual patterns trump averages.8
In other words: you can track your phases for self-awareness, but science doesn’t yet back the idea that you’ll train better or worse depending on the day of your cycle.
Oral Contraceptives and Exercise Performance
What about women on hormonal birth control; does the pill flatten or hinder performance?
Elliott-Sale et al., 2021 (Sports Medicine): On average, oral-contraceptive users perform about the same as non-users. Any differences are “trivial” and vary widely from person to person.9
Nolan et al., 2024 (Sports Medicine): Found no significant differences in hypertrophy, power, or strength gains after resistance training between users and non-users.10
Dalgaard et al., 2019 & 2022: In both untrained and trained women, oral contraceptives did not blunt muscle growth or strength gains.11
Glenner-Frandsen et al., 2023 (Sports Health): Detected slightly slower recovery markers after muscle-damage protocols among monophasic-pill users, but sample sizes were small and findings context-specific.12
Taken together, this body of evidence supports an N=1 approach13: your response may differ, but on average, the pill doesn’t make or break athletic progress.
The Bigger Picture
As summarized by Beyond the Menstrual Cycle14, focusing narrowly on “phase-based” prescriptions may miss the point. Most experts now advocate symptom-led training, adjusting workouts for how you actually feel, not what a chart says.
Media outlets echo that stance:
TIME15 and Clue/Oxford16 caution that “balancing your hormones” through cycle syncing is more marketing than medicine.
Tom’s Guide 2025 expert roundup17 reminds readers that research simply doesn’t support precise syncing yet.
The Bottom Line
Cycle syncing is built on a biologically sound premise–hormones do influence how you feel and perform–but the current science doesn’t justify prescriptive lifestyle changes by phase.
You can absolutely use your cycle as a tool for body awareness, noting patterns in energy, appetite, or focus. Just don’t treat it like a training plan carved in stone.
If tracking helps you feel more connected to your body, great. If not, know that your physiology is already doing a pretty incredible job on its own.
So… Cycle Syncing vs Birth Control
Let’s zoom out. If cycle syncing is about working with your hormones, hormonal birth control is about managing them. How do the tradeoffs stack up?
Pros and Cons of Birth Control
Pregnancy Prevention
We can’t talk about Birth Control without first addressing that it is highly effective for pregnancy prevention. I will dive into this more in the later section regarding how one can still have birth control if not on Birth Control, but artificial contraceptives are the most effective form of birth control when used correctly.
Cancer Risk
Hormonal contraceptives (HCs) are associated with a small but significant increase in breast cancer risk that diminishes after discontinuation18. However, there is a much larger decrease in ovarian19 and endometrial20 cancers. Large-scale studies have shown that long-term use of birth control may reduce ovarian cancer risk by up to 50% and endometrial cancer risk also declines significantly. (And another source just for fun.21)
Bone Health
For adult women, combination oral contraceptives appear neutral to slightly beneficial for bone mineral density (BMD), especially post-adolescence.22
Blood Clots (VTE)
Combination HCs increase the risk of venous thromboembolism (VTE), though the absolute risk remains low-especially compared to pregnancy23 (pregnancy significantly increases the risk of VTE).
Ischemia Stroke (IS)/Myocardial Infarction (MI)
A Danish registry study found low but real increases in risk of IS/MI, primarily in smokers and older women.24
Mood-Related Effects
Most users report no mood change, but a subset–especially adolescents or those sensitive to hormonal shifts–experience mood disturbances such as depression, anxiety, or irritability. But even while some HCs (“for some women, in some contexts, using some HCs”) can increase the risk of depression, “some HCs can be effective in treating depression.”25
References:
Mengelkoch et al., 2025 (Contraception): No significant increase in depression for adult users.
Skovlund et al., 2016 (Epidemiology and Psychiatric Sciences): Danish cohort found higher depression risk among adolescent users.26
Wit et al., 2021 (BJPsych Open): HCs do not lead to an increase in depressive symptoms in adult women.27
Libido Changes?
Libido changes are highly individual. Some report dips, others increases, and research hasn’t pinpointed consistent predictors.28
Changes in Attraction or Partner Preference?
The myth that the pill changes who you are attracted to has been widely circulated. Early small studies29 hinted at this, but larger, better-controlled research30 doesn’t support it.
Management of Hormonal Conditions
HCs can reduce symptoms of acne3132, Premenstrual Syndrome (PMS), Premenstrual Dysphoric Disorder (PMDD)33, and polycystic ovary syndrome (PCOS)3435 by stabilizing hormonal fluctuations.
(If you view this section’s claim as a band-aid and not a solution, you are somewhat right. But what someone chooses to do is very situationally dependent. Trying to figure out root cause can involve metabolic workups, nutritional adjustments, lifestyle interventions, therapy or other medication, or functional medicine (though evidence for these varies). Some people may just want relief).
Bottom Line
For most women, hormonal birth control is safe and effective, offering real health benefits that outweigh risks when prescribed thoughtfully.
The risks–especially for mood and cardiovascular side effects–are individual, not universal.
I found an interesting chart from the CDC36 that outlines eligibility criteria for different contraceptives depending on what condition you may have (everything from age to depression to hypertension). This is a great way to quickly assess the likelihood of adverse effects depending on your unique factors. (The chart is based on this research.37)
Can you cycle sync while on birth control?
Because HCs suppress natural ovulation and regulate hormone levels, they flatten the cyclical hormonal fluctuations that “cycle syncing” relies on. So, while you can still use elements of body awareness–like mindful rest, nutrition, or exercise tracking–the traditional four-phase syncing model I discussed previously doesn’t apply in the same way while on birth control.
How to “birth control” while cycle syncing
I grew up Catholic where Natural Family Planning (NFP)--also known as Fertility Awareness-Based Methods (FABMs)--was part of how we talked about sexual health and family planning. The Catholic Church opposes artificial contraception and promotes NFP as the only moral way to regulate birth.
So I learned the basics: taking your temperature daily to detect the small rise that occurs after ovulation (the signal that you’re either entering or exiting your fertile window), a general understanding of fertile windows, and that none of these FABMs protect against STIs. There was some mention of checking cervical mucus, though I doubt our classroom ever went into much detail.
Regardless of your stance on religion or the morality of contraception, the concept behind NFP always made scientific sense to me, so I filed it away for when I might want to become a mom.
When I later heard about cycle syncing, which also involves tracking your cycle to better align with your body, it struck me as a kind of secular cousin to NFP. But the similarity ends at awareness. Cycle syncing isn’t designed to track fertility signs precisely enough to predict ovulation or prevent pregnancy. (Some proponents of cycle syncing do go into precise detail about fertility signs, but there’s no standardized method or scientific rigor behind it.)
By contrast, NFP and FABMs are evidence-based methods that rely on measurable biomarkers (basal body temperature, cervical mucus, and luteinizing hormone (LH) surges) to identify fertile and infertile days. Depending on how they’re used, these methods can help either achieve or avoid pregnancy.
With content gathered from this research.383940
And, What Am I Going to Do?
After weeks of research and more late-night PubMed tabs than I care to admit, here’s where I’ve landed:
Cycle Syncing sounds empowering - and in some ways, it is. Paying attention to your energy, sleep, and cravings can absolutely make you feel more connected to your body. But there’s no single formula or proven system that will guarantee balance, happiness, or health. What’s sold as science is often, at best, personalized mindfulness with a menstrual calendar. If that works with you, great! If it doesn’t, that’s okay too.
Hormonal birth control, on the other hand, is one of the most studied medical interventions in history. It’s not perfect–no medication is–but for most people, it’s safe, effective, and even protective in certain ways. It also comes with tradeoffs: possible mood shifts, libido changes, or simply the unease of not knowing your “natural” rhythm.
Here’s what feels true for me:
I like having control. I like the predictability of not having a period. I like that modern medicine gives me that option–and I like that I can still be informed enough to question it.
I don’t think the takeaway should be choosing between “natural” and “medical.” I can be both scientifically curious and self-aware.
The real lesson here? You don’t need to rebuild your entire life around your uterus to be “in tune” with your body.
You just need to listen–with curiosity, compassion, and common sense–and do what feels right for you. That answer will look different for everyone.
I’m lucky enough to be, as I like to call it, scientifically average–no major hormonal issues, everything generally within range. I can’t speak for anyone else, because everyone’s body tells a different story. Maybe that story involves cycle syncing (the Balanced Beyars sure think so). Maybe it means staying on birth control (that’s me, for now). Neither one of us is wrong, we’re each right for ourselves.
I am a big believer in learning to read your own body. If cycle syncing sparks your curiosity and you’d like to explore it further, here’s a list of books that are often recommended. I haven’t personally read them yet, so consider this a starting point rather than an endorsement:
The Fifth Vital Sign
In the FLO
Fix Your Period
Period Power
The Hormone Cure
WomanCode
Taking Charge of Your Fertility
The Happy Hormone Guide
Beyond the Pill
https://pmc.ncbi.nlm.nih.gov/articles/PMC5691553/
https://www.mdacne.com/questions/how-does-the-skin-change-during-the-menstrual-cycle
ttps://www.ucl.ac.uk/news/2024/may/female-athletes-more-likely-get-injured-certain-points-their-menstrual-cycle
https://www.forbes.com/health/womens-health/cycle-syncing/
https://pubmed.ncbi.nlm.nih.gov/32661839/
https://www.frontiersin.org/journals/sports-and-active-living/articles/10.3389/fspor.2023.1054542/full
https://pmc.ncbi.nlm.nih.gov/articles/PMC8053180/
https://hsph.harvard.edu/research/apple-womens-health-study/study-updates/exploring-exercise-habits-by-menstrual-cycle-phase/
https://pmc.ncbi.nlm.nih.gov/articles/PMC8053180/
https://link.springer.com/article/10.1007/s40279-023-01911-3
https://pmc.ncbi.nlm.nih.gov/articles/PMC6614284/
https://journals.sagepub.com/doi/abs/10.1177/19417381221121653
https://statisticseasily.com/glossario/what-is-n-1-analysis-understanding-individual-data/
https://ijspt.scholasticahq.com/article/126285-beyond-the-menstrual-cycle-time-for-a-holistic-approach-to-athlete-health-and-performance
https://time.com/6277941/balance-hormones-cycle-syncing-myth/
https://www.allure.com/story/clue-study-period-syncing-myth
https://www.tomsguide.com/wellness/fitness/top-experts-debunk-the-cycle-syncing-trend-the-evidence-just-isnt-there
https://pmc.ncbi.nlm.nih.gov/articles/PMC10705112/
https://pubmed.ncbi.nlm.nih.gov/18294997/
https://pubmed.ncbi.nlm.nih.gov/26254030/
https://www.pharmacytimes.com/view/balancing-cancer-risks-and-benefits-of-oral-contraceptives
https://link.springer.com/article/10.1007/s10654-025-01273-2
https://pubmed.ncbi.nlm.nih.gov/24030561/
https://www.tctmd.com/news/danish-analysis-updates-stroke-and-mi-risks-contemporary-contraceptives
https://www.uclastresslab.org/pubs/Mengelkoch_Contraception_2025.pdf
www.cambridge.org/journals/epidemiology-and-psychiatric-sciences/article/population-based-cohort-study-of-oral-contraceptive-use-and-risk-of-depression/B3C611DD318D7DC536B4BD439343A5BD
https://pmc.ncbi.nlm.nih.gov/articles/PMC8220855/
https://pmc.ncbi.nlm.nih.gov/articles/PMC8836660/
https://pubmed.ncbi.nlm.nih.gov/23528282/
https://journals.sagepub.com/doi/10.1177/0956797618760197
https://pmc.ncbi.nlm.nih.gov/articles/PMC5925193/
https://pmc.ncbi.nlm.nih.gov/articles/PMC11785877/
https://pmc.ncbi.nlm.nih.gov/articles/PMC6759213/
https://academic.oup.com/jcem/article-abstract/100/3/794/2838953
https://www.asrm.org/practice-guidance/practice-committee-documents/recommendations-from-the-2023-international-evidence-based-guideline-for-the-assessment-and-management-of-polycystic-ovary-syndrome/
https://www.cdc.gov/contraception/media/pdfs/2024/07/us-mec-summary-chart-color-508.pdf
https://www.cdc.gov/mmwr/volumes/73/rr/rr7304a1.htm
https://pmc.ncbi.nlm.nih.gov/articles/PMC9171018/
https://www.aafp.org/pubs/afp/issues/2012/1115/p924.html
https://www.guttmacher.org/sites/default/files/factsheet/contraceptive-effectiveness-united-states.pdf